Coughing, Sneezing, Wheezing, and Panting: What Is Normal and What Is Not
Pets make all kinds of sounds. A quick sneeze after nosing through a pile of leaves, a snort when they get too excited greeting you at the door, a brief cough after gulping water too quickly, or a funny snore while dreaming. Most of the time, these pass without a second thought. But when respiratory sounds become frequent, get louder over time, or show up alongside other symptoms, they are often a signal that something real is going on, and knowing which sounds fall into the “wait and see” category versus the “let’s go right now” category can make a meaningful difference for your pet.
At El Paso Animal Hospital, we handle urgent and emergency cases during open hours and can begin stabilization with oxygen, IV fluids, and medication while we work through what is causing the problem. Our in-house diagnostics allow us to run bloodwork and take chest radiographs quickly, so treatment does not have to wait. If your pet’s breathing is worrying you, call us at 316-788-1000 while you are on the way so we can be ready when you arrive.
Coughing in Dogs and Cats
Not every cough looks or sounds the same, and the character of the cough is often the first clue toward figuring out what is behind it.
Dry, Honking Cough After Social Exposure
If your dog has been to boarding, daycare, or the dog park recently and comes home with a forceful, honking cough that gets worse with activity or a collar pull, kennel cough (infectious tracheobronchitis) is high on the list. It spreads easily in shared spaces and is usually self-limiting, but it warrants a call if lethargy or a high fever develops alongside it.
Honking Cough in a Small Dog
A goose-honk cough that appears during excitement or when a collar puts pressure on the neck is a hallmark of collapsed trachea, a condition where the cartilage rings supporting the windpipe weaken over time. It is most common in small breeds like Yorkshire Terriers, Chihuahuas, and Pomeranians. Switching to a harness removes collar pressure from the equation entirely, and medical management or surgery can improve quality of life in affected dogs.
Wet, Gurgly, or Productive Cough
A moist, bubbling cough, particularly in an older dog or one with reduced energy and exercise tolerance, raises concern for fluid in the lungs from pneumonia, aspiration, or heart disease. If your dog’s cough seems to worsen when lying down at night or after a walk that would not have slowed them down before, that pattern deserves same-day attention.
Cough That Does Not Resolve With Standard Treatment or Time
A cough that persists despite antibiotics or fails to follow the expected timeline of an infectious illness can indicate something structural going on. Masses in the chest and lung involvement from cancer can produce coughing, weight loss, and exercise intolerance that does not respond the way an infection would. Our diagnostic imaging allows us to assess the chest and pursue answers when the straightforward explanations are not fitting.
Panting in Cats: Always Worth Paying Attention To
Dogs pant. That is normal and expected. Cats do not, at least not under normal circumstances. A cat panting while resting, after minor activity, or in a comfortable environment is telling you something is wrong. The list of causes includes respiratory disease, heart disease, pain, extreme stress, and heatstroke, none of which should be left unaddressed. A cat with mouth-open breathing, rapid visible chest movement, or a stretched neck posture needs to be seen the same day.
Crouched Cat, Neck Extended, Breathing Hard
When a cat is having an asthma episode, the posture is recognizable: crouched low, neck stretched forward, breathing with visible effort and sometimes open-mouthed. An active asthma attack in a cat is a genuine emergency, not a wait-until-tomorrow situation.
Sneezing and Nasal Discharge
One sneeze after sniffing something dusty is not worth worrying about. Repeated sneezing, especially with discharge of any color, is a different story.
Repeated Sneezing With Colored Discharge
Yellow or green nasal discharge points toward secondary bacterial involvement and is most commonly associated with feline upper respiratory infection in cats, or bacterial rhinitis in dogs. These infections are particularly common in cats coming from shelters or with outdoor access, and the FVRCP vaccine offers protection against the most common viral triggers.
Sudden, Dramatic Sneezing Fits With Pawing at the Face
If sneezing comes on suddenly and intensely, particularly after outdoor time in areas with dry grasses and weeds, a foxtail or grass awn lodged in the nasal passage is a real possibility. These plant fragments are barbed, move in one direction, and do not come out on their own. Removal requires sedation, and the sooner it happens, the better. A nosebleed paired with sneezing is never something to wait on, as it can indicate immune-mediated disease or a nasal mass in addition to a foreign body.
Persistent Sneezing in a Young Cat That Is Not Responding to Treatment
Nasopharyngeal polyps are benign growths that develop in the nasal passage or middle ear in cats and are more common in younger animals. They produce chronic sneezing, nasal discharge, noisy breathing, and sometimes a head tilt, and they are frequently mistaken for a respiratory infection that just will not clear. Surgical removal is typically curative.
Sneezing With a Known Dental History
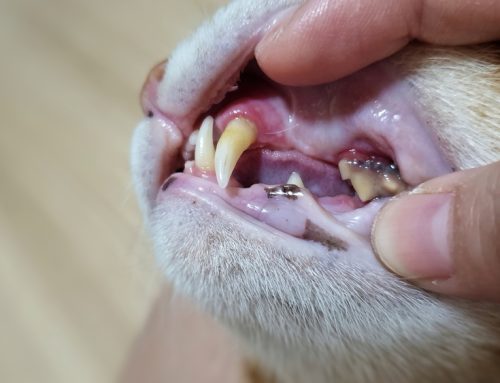
The roots of the upper teeth sit remarkably close to the nasal passage. When upper tooth root infections erode through that boundary, chronic nasal discharge and sneezing follow, and standard respiratory treatments do nothing to fix it. If your cat or dog has a history of dental disease and ongoing nasal symptoms, that connection is worth exploring with professional dental care.
Reverse Sneezing
Few things are more alarming to witness the first time than reverse sneezing. The rapid, repeated snorting inhalations look terrifying and sound like the dog is choking. In reality, it is usually a benign spasm of the soft palate triggered by an irritant, lasts under a minute, and resolves without intervention. It is particularly common in small breeds and brachycephalic dogs.
If your pet has an episode, record it on your phone. That video helps us distinguish reverse sneezing from actual respiratory distress at a glance, which is genuinely useful clinical information.
Snoring, Snorting, and Noisy Breathing
Some dogs snore. It is endearing right up until it is not. Snoring that has been present since puppyhood in a flat-faced breed is a different clinical picture than new-onset snoring in a dog that previously breathed quietly, and the latter deserves investigation.
Brachycephalic obstructive airway syndrome (BOAS) affects dogs and cats with compressed facial anatomy, including Bulldogs, Pugs, French Bulldogs, Boston Terriers, and Persian cats. The narrowed nostrils, elongated soft palate, and sometimes narrowed trachea that come with flat-faced breeds create chronic airway restriction that worsens with heat, obesity, excitement, and age. These pets work much harder to breathe than their easygoing expressions suggest, and surgical correction of the anatomical components significantly improves their quality of life and long-term respiratory health.
Stridor: The Raspy Sound on the Inhale
Stridor is a coarse, raspy sound that occurs on inhalation and points toward obstruction at the level of the larynx (voice box) or upper airway. Laryngeal paralysis is the most common cause in older large-breed dogs, particularly Labrador Retrievers and Golden Retrievers. The cartilages that should open the airway on inhalation stop moving as they should, progressively narrowing the airway over time. Voice changes and exercise intolerance usually accompany the noise. Surgical correction, called arytenoid lateralization, is effective and improves breathing considerably.
Wet, Gurgling, or Fluid-Filled Breathing Sounds
A moist, bubbling quality to breathing indicates fluid in or around the lungs. Pneumonia produces wet respiratory sounds alongside coughing, fever, and lethargy. Congestive heart failure causes pulmonary edema (fluid accumulation in lung tissue) that makes breathing progressively more labored, often worst at night and at rest.
Either presentation with visible respiratory effort, blue or gray gums, or collapse is an emergency that requires immediate care.
When Breathing Is an Emergency
Respiratory distress does not wait, and neither should you. Come in immediately, calling 316-788-1000 on the way, for any of the following:
- Cyanosis: blue, gray, or very pale gums indicating the blood is not carrying adequate oxygen
- Open-mouth breathing in a cat at rest
- Breathing that involves visible belly movement, extended neck posture, or splayed elbows
- Rapid breathing at rest; respiratory rates over 40 breaths per minute while sleeping are cause for concern
- Coughing that will not stop or produces blood
- Collapse associated with any respiratory sign
- Sudden facial or throat swelling, hives, vomiting, or difficulty breathing immediately after a vaccine, insect sting, or exposure to a new food or medication. These are signs of anaphylactic shock, which can rapidly progress to airway swelling and cardiovascular collapse
These presentations require immediate evaluation, not a callback queue. Our urgent and emergency care is available during open hours, and calling ahead while you are driving in gives us time to prepare.
How We Diagnose Respiratory Symptoms
When your pet arrives with breathing concerns, we move quickly. We immediately triage your pet and begin stabilization with oxygen therapy, IV fluids, and medications to help them breathe better while we begin the diagnostic process.
Physical Examination
Auscultating the lungs and heart with a stethoscope identifies wheeze, crackle, and fluid. Tracheal palpation identifies sensitivity. Gum color and pulse quality give us an immediate read on cardiovascular status before diagnostics begin.
Diagnostic Workup
- Bloodwork: A complete blood count and chemistry panel screen for infection, anemia, organ function, and metabolic contributors. Heartworm testing is included when cardiac involvement is suspected, as heartworm disease affects both the lungs and heart and is present in Kansas.
- Chest radiographs: Our in-house imaging evaluates lung fields, heart size, and major airway structures, providing answers without a referral visit.
Treatment
Treatment follows the diagnosis. We’ll go over what we found, discuss the possible solutions, and formulate a plan together. This might include antibiotics for bacterial infection, bronchodilators and anti-inflammatory medications for asthma, diuretics and cardiac medications for heart failure, or surgical correction for structural airway disease, including brachycephalic anatomy and laryngeal paralysis.
Getting Ahead of Respiratory Problems
Some respiratory conditions are not preventable, but many can be caught early or avoided altogether with consistent care.
Stay current on vaccinations. Kennel cough and canine influenza spread easily in boarding, daycare, and dog park settings. If your dog has regular social exposure, ask us about whether influenza vaccination makes sense given their lifestyle.
Keep up with heartworm and parasite prevention. Heartworm disease damages both the lungs and the heart, producing coughing and exercise intolerance that worsens over time. Year-round preventative care is the most reliable way to keep it out of the picture entirely.
Address dental disease proactively. The connection between dental health and respiratory symptoms is easy to miss until it is causing a problem. Upper tooth root infections can erode into the nasal passage and produce chronic discharge that does not respond to standard respiratory treatment. Consistent dental care prevents that pathway from developing.
Switch flat-faced and small dogs to a harness. Collar pressure on the trachea aggravates tracheal collapse in small breeds and adds unnecessary strain in any brachycephalic dog. A well-fitted harness removes that pressure entirely.
Schedule regular wellness exams, especially in senior pets. A heart murmur, subtle lung crackle, or mildly elevated resting respiratory rate may be the earliest sign of a developing condition. Catching these findings at a senior wellness visit creates the opportunity to manage a condition before it reaches a crisis point. Screening senior pets for early heart disease is a routine and meaningful part of what we do, because the earlier it is identified, the more options there are.
Have brachycephalic pets evaluated before symptoms become severe. Flat-faced dogs benefit from an airway evaluation early in life. Surgical correction of BOAS anatomy produces better outcomes when performed in a young, healthy dog than when delayed until breathing difficulty is significant. El Paso Animal Hospital handles a wide range of complex surgical needs, with careful anesthetic monitoring for patients with airway problems.

Frequently Asked Questions
My dog has been coughing for a few days but seems otherwise fine. Should I bring them in?
Yes. A cough that has persisted beyond 48 hours warrants evaluation, even without other obvious symptoms. Coughs can be the first sign of infections, structural problems, or cardiac disease that benefit from early diagnosis. Give us a call and we will figure out the right next step together.
My cat coughed once and it has not happened again. Do I need to worry?
A single isolated episode is less concerning than recurrent ones. Keep an eye on it. If it happens again, or if you notice any change in breathing posture, energy level, or appetite alongside it, call us.
How do I know if my pet is breathing too fast?
Count the rise and fall of the chest while your pet is relaxed or asleep. Count for 30 seconds and double the number. A resting respiratory rate above 30 breaths per minute, or one that is noticeably higher than your pet’s usual baseline, is a reason to reach out to us the same day.
Can I wait and bring my pet to a regular appointment?
If your pet has labored breathing, is breathing with visible effort, or is a cat breathing with its mouth open, do not wait. For persistent but less acute symptoms, like a cough that has been present for a few days, call us so we can help you decide. We would always rather hear from you and tell you it can wait than have you wait when it cannot.
Your Pet’s Breathing Deserves a Closer Look
Respiratory symptoms in pets range from entirely harmless to immediately life-threatening, and the difference is not always obvious from the outside. At El Paso Animal Hospital, our team brings over 150 years of combined experience to urgent and emergent cases, and our diagnostic capabilities allow us to move quickly from question to answer to treatment when time matters.
If your pet’s breathing has changed, do not sit on it. Contact us or call 316-788-1000. Walk-ins are welcome, and calling ahead while you are on the way gives our team time to prepare for your arrival.








Leave A Comment